| J Korean Dent Assoc > Volume 62(6); 2024 > Article |
|
Abstract
The identification of the facial nerve trunk(FNT) is an important step in surgical procedures involving the parotid gland and adjacent structures to minimize the risk of inadvertent nerve damage which leads to facial muscle paralysis. Despite the availability of various anatomic landmarks such as the tragal pointer, posterior belly of digastric muscle, tympanomastoid suture, digastric branch of facial nerve and styloid process, no single landmark is perfect, with variations observed between individuals. Therefore, a comprehensive knowledge of facial nerve anatomy is essential for FNT identification. In this review, we tried to introduce clinically meaningful methods for the localization of facial nerve trunk. The preference of landmark could be changed by the major of the surgeon or the location of the tumor of the patients. Understanding the characteristics and drawbacks of the landmarks and choosing multiple landmarks that were convenient for surgeon would be necessary.
The facial nerve, the 7th cranial nerve, carries nerves involved in facial expression, taste perception for the anterior 2/3 of the tongue, tear production, and moderating sensitivity to noise volume by controlling the stapedius muscles. After emerging from the base of the skull through the stylomastoid foramen(SMF), the facial nerve gives rise to the posterior auricular nerve and the digastric nerve. The main trunk of the nerve then continues anteriorly and inferiorly into the parotid gland, where it bifurcates into upper and lower divisions. Subsequently, it splits into five branches(temporal, zygomatic buccal, marginal mandibular and cervical), responsible for innervating the muscles of facial expression. The portion of the nerve that extends from the SMF to the bifurcation is commonly known as the facial nerve trunk(FNT).
The identification of FNT is a crucial step in parotid surgery because inadvertent damage to the nerve can result in paralysis of half of all the facial muscles of expression, leading to cosmetic deformity, psychological trauma and corneal irritation form lack of motor function [1]. Common anatomic landmarks that can indicate the position of FNT include the tragal pointer, posterior belly of digastric muscle, tympanomastoid suture, stylomastoid artery, styloid process and posterior auricular artery [2,3]. However, none of these landmarks are perfect, and there can be variations between individuals and even between living patients and cadavers [4]. Therefore, a comprehensive knowledge of its anatomy, meticulous dissection and experience are the keys for identification of FNT. The purpose of this review is to provide an overview of the landmarks and methods for the identification of FNT during surgery or anatomic dissection.
There are osseous and soft tissue landmarks in identification of FNT. Well-known bony landmarks include the tympanomastoid suture, mastoid process, C1 transverse process and styloid process. Soft tissue landmarks include the posterior belly of digastric muscle and the tragal pointer(Fig. 1).
The tragal pointer is the anterior/inferior tip of the tragus portion of the external ear cartilage(Fig. 2). The anterior/inferior part of the tragus, named ŌĆśpointerŌĆÖ, takes a bluntly pointed shape, directing anterior, inferior and deep to the superficial surface of the preauricular area [5]. It is a widely used landmark, with FNT typically located around 1cm deep and inferior to the pointer. Additionally, the direction of the tragal cartilage is indicative of the location of the facial nerve. However, the tragal pointer has a blunt, asymmetric and variable tip that can change with retraction, resulting in significant variation in distances from the pointer to the facial nerve [6]. The mean distance from tragal pointer to FNT ranges from 6.37 to 34mm with the overall average of 13.60┬▒11.00mm [3]. A study compared the cadaver and live patients reported a longer distance in cadaver(13.04 ┬▒ 5.238mm) than live patients(9.95 ┬▒ 3.967mm) with a statistically significant difference(p = 0.036) [4]. Considering the direction of the pointer, 20 percent of the pointer pointed to FNT [7]. Nevertheless, due to its ease of dissection, superficial position and reproducibility, the tragal pointer is still routinely used with other landmarks in the identification of FNT.
During parotidectomy, lateral retraction of the sternocleidomastoid muscle reveals the posterior belly of digastric muscle. This muscle is easily identifiable due to its location and the orientation of muscle fibers, which extend towards the mastoid tip. FNT lies deeper than this plane and runs approximately 1cm above and parallel to the upper border of the digastric muscle near its insertion point at the mastoid tip [8]. Therefore, the upper border of the muscle near the attachment of the mastoid process has frequently been utilized as a landmark for identifying FNT. The mean distance from the digastric muscle ranges from 4.5 to 14.6 with an average of 8.79 ┬▒ 3.99mm [3] and Shah et al, reported that the mean distance was similar in cadaver and live patients [4]. Due to its proximity to FNT, minimum anatomical variation, ease of dissection, and exposure during parotidectomy, the posterior belly of digastric muscle is still used as a landmark along with the tragal pointer [3].
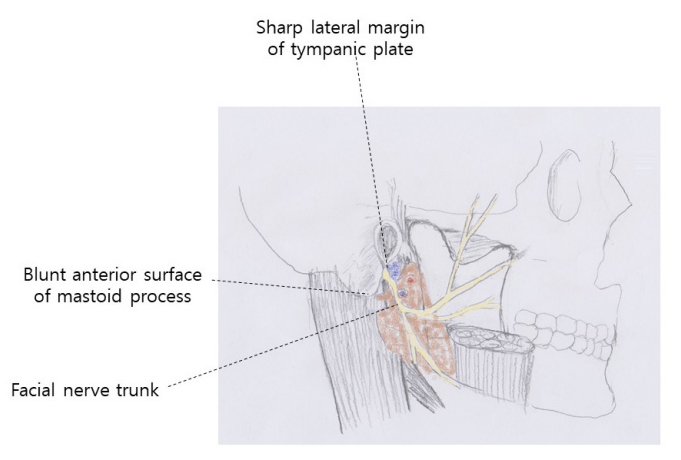
The tympanomastoid suture is a bony landmark for identifying FNT. Brintnall et al. described the identification method of FNT using the tympanomastoid suture [9]. Dissection proceeds deeply in the zone behind the parotid gland and close to the cartilaginous ear canal. Between two bony prominences, 1) superiorly, the sharp, fingernail-like bony ridge at the anteroinferior margin of the external auditory meatus of the skull, and 2) inferiorly, the broad blunt anterior margin of the mastoid process of the temporal bone, there is a V-shaped sulcus. The nerve cannot be more than 2 to 3 mm from the depth of the dissection in a pad of loose areolar tissue(Fig. 3). FNT will be exposed by gently spreading the areolar tissue.
The use of tympanomastoid suture as a landmark is controversial. Osseous landmarks are known to be more reliable because of their rigidness. It is a convenient landmark for otolaryngologists who encounter it regularly in tympanoplastic surgery [1]. Additionally, the distance to FNT is shorter than other landmarks and there were no significant differences between live patients and cadavers and its relation to the nerve is reliable because it leads to the stylomastoid foramen(Fig. 4) [4]. The tympanomastoid suture can be identified in cadavers without much difficulty. However, in surgery, this requires dissection to the periosteum of the fissure, adding unnecessary complexity [10]. If the periosteum is not dissected, it is essentially a palpable landmark and direct visualization of the suture is practically not possible [8]. Furthermore, it is a comparatively deeper structure, requiring comprehensive digital palpation for its exact identification [10].
Previous landmarks could be classified as quantitative landmarks as they were based on their distance to FNT, while the digastric branch of the facial nerve(DBFN) could be described as a qualitative landmark. Quantitative landmarks may be unreliable in patients whose anatomy and measurements differ from known measured distances. In such cases, following qualitative landmarks can lead to FNT, because of their direct anatomic relationship with FNT [11]. DBFN is the second branch of the extratemporal FNT. After exposing the posterior belly of digastric muscle and separating the insertion of the sternocleidomastoid muscle(SCM) onto the tip of the mastoid process to expose the mastoid tip, superomedial aspect of the posterior belly of digastric muscle was evaluated to find the point of innervation by DBFN. Then, DBFN was retrogradely dissected until the identification of its main trunk [11,12]. The insertion point of DBFN onto the posterior belly of digastric muscle was located on the superomedial aspect of the muscle with a distance of 13.6 ┬▒ 2.0mm(range: 10~17mm) from the tip of the mastoid process. Anterior and medial to DBFN, the stylomastoid artery was accompanied [11]. Although DBFN seemed reliable and consistently identified at the estimated location, only a few studies have been reported and the major anatomical study by Meybodi et al.(2019) [11] was limited to cadaveric study. The fact that DBFN accompanies the artery may cause unexpected bleeding. Therefore, inexperienced surgeons need caution when using this landmark.
The styloid process, a bony landmark, lies deep to the facial nerve. Therefore, when the surgeon reached the styloid process, the nerve has already been passed. Additionally, the accuracy of this landmark is compromised due to the cases of elongation, calcification of the stylohyoid ligament or absence [7].
Due to the lack of consensus on the best single landmark to use, it is now becoming standard to utilize multiple landmarks when identifying and locating FNT [5].
Using tragal pointer and posterior belly of digastric muscle is the most widely used method. After incision, the cartilage of the pointer is followed medially. The tragal pointer is located superficially to the main trunk of the facial nerve and points to the deeply located main trunk, thereby indicating that FNT is near. Then, the junction of the posterior belly of the digastric muscle and SCM is used for FNT identification. This junction is located approximately 4mm inferior to FNT and at the same depth as the main trunk. Then, FNT can be located using a nerve stimulator when approaching this junction [3].
The dissection method of posterior belly of digastric muscle is as following. The tail of the parotid gland is located at the anterior border of SCM. The tail of the parotid gland is separated from SCM and from the cartilaginous external auditory canal. The greater auricular nerve was divided as close to the parotid gland as possible to preserve the posterior branch. The parotid gland is retracted medially and blunt dissection is performed to the posterior border of the gland. Then, SCM is retracted posteriorly and the posterior belly of digastric muscle will be visualized [13]. Tracing the posterior belly of digastric muscle upwards and backwards to the mastoid process will encounter the FNT.
Some authors introduced methods for identifying FNT using the tympanomastoid suture, posterior belly of digastric muscle and tragal pointer, together during parotid surgery [4,14,15]. The dissecting methods until the tragal pointer and the posterior belly of digastric muscle are the same as described previously, and the tympanomastoid suture serves as a more specific guide to locate FNT. Between the tragal pointer and the superior border of the posterior belly of digastric muscle, deeper to the level of these landmarks, the tympanomastoid suture is palpable. This region containing tympanomastoid suture is identified as the ŌĆ£valleyŌĆØ of the nerve and FNT would be found a few millimeters inferiorly at this leve [l4,14]. Using tympanomastoid suture is controversial as described previously. This method can be useful in cases where it is difficult to find facial nerves due to recurrence or surrounding lesions.
Borle et al. proposed an anatomical triangle for ease of identification of FNT [13]. Briefly, the first line starts from the tip of the mastoid process, along the superior border of the posterior belly of digastric muscle. The second line is drawn along the posterior border of the ramus after palpation. The third line runs anteriorly from the tip of the mastoid process until it joins the second line along the posterior border of the ramus(Fig. 5). FNT is often found within this triangle, just above the angle formed at the tip of the mastoid process with blunt dissection. The mean distance of FNT from the angle of mastoid process tip was reported as 12.18 ┬▒ 2mm(range 9~15mm). This method uses another landmark, the posterior border of the ramus, but it is similar to existing methods in the concept of finding FNT around the mastoid process.
In this review, we tried to introduce clinically meaningful methods for the localization of facial nerve trunk. The tragal pointer, the posterior belly of digastric muscle and the tympanomastoid suture are the most frequently described landmarks in literature. However, no single landmark is best to use and it has now become standard practice to utilize multiple landmarks. The preference of landmark could be changed by the major of the surgeon or the location of the tumor of the patients. Accurate knowledge of the anatomy and combining these landmarks which were convenient to surgeon would minimize the risk of nerve injury and achieve optimal surgical outcomes.
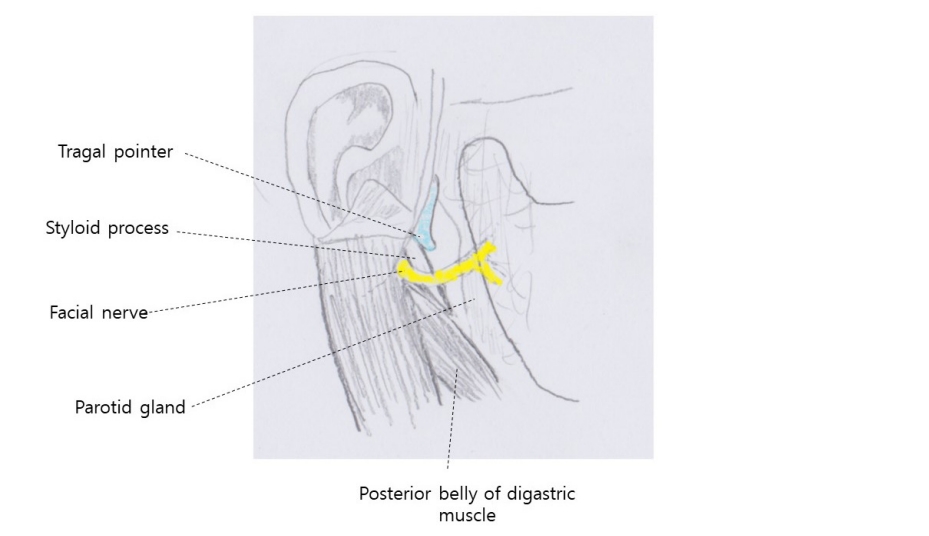
Figure┬Ā2.
Relation of facial nerve trunk with tragal pointer and the posterior belly of digastric muscle. Facial nerve trunk is known to lie around 1 cm deep and inferior to the pointer. The part of the tragal cartilage is known to direct the facial nerve. As for the digastric muscle, facial nerve trunk runs approximately 1 cm above and parallel to the upper border of the digastric muscle near its insertion point at the mastoid tip.
Figure┬Ā3.
Two bony landmarks utilized to locate the ŌĆśpalpable sulcusŌĆÖ in which the trunk of the facial nerve is found.
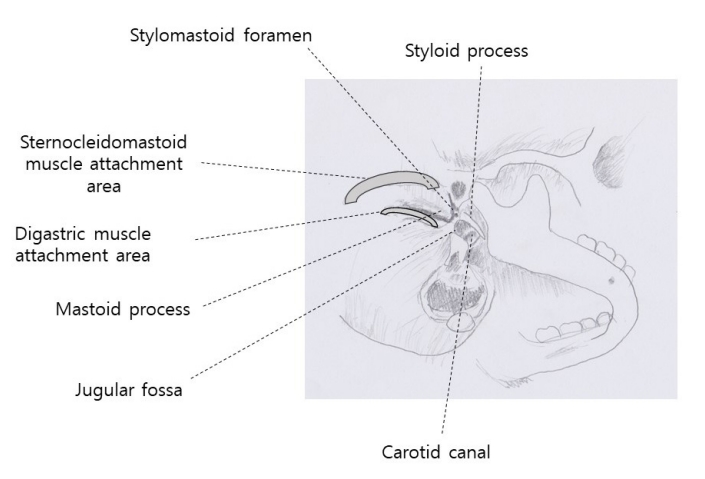
Figure┬Ā4.
Skeletal bed of the facial nerve from an inferior view. The region containing the tympanomastoid suture extends to the stylomastoid foramen.
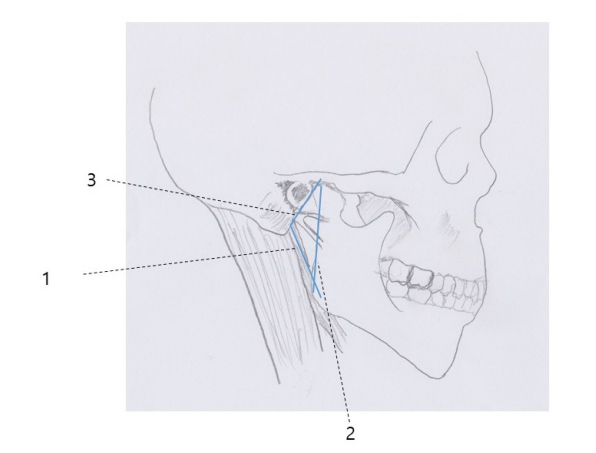
Figure┬Ā5.
The anatomical triangle for the identification of the facial nerve trunk. The first line (1) extends from the tip of the mastoid process along the superior border of the posterior belly of digastric muscle. Second line (2) is drawn along the posterior border of the ramus after palpation. The third line (3) runs anteriorly from the tip of the mastoid process, until it joins line 2 along the posterior border of the ramus. The facial nerve trunk is commonly located within this triangle, just above the angle formed by line 1and 3.
REFERENCES
1. Tabb HG, Scalco AN, Fraser SF. Exposure of the facial nerve in parotid surgery. (Use of the tympanomastoid fissure as a guide). Laryngoscope 1970;80:559ŌĆō67. https://doi.org/10.1288/00005537-197004000-00004.


2. Elvan O, Bobus A, Erdogan S, Aktekin M, Olgunus ZK. Fetal anatomy of the facial nerve trunk and its relationship with posterior auricular artery. Surg Radiol Anat 2019;41:153ŌĆō9. https://doi.org/10.1007/s00276-018-2126-x.


3. Ji YD, Donoff RB, Peacock ZS, Carlson ER. Surgical Landmarks to Locating the Main Trunk of the Facial Nerve in Parotid Surgery: A Systematic Review. J Oral Maxillofac Surg 2018;76:438ŌĆō43. https://doi.org/10.1016/j.joms.2017.06.039.


4. Shah AS, Nair S, Pavithra V, Aishwarya JG, Brijith KVR, Thakur D. Anatomical and Surgical Study to Evaluate the Accuracy of "C-M-S" Technique in Facial Nerve Identification During Parotid Surgery. Indian J Otolaryngol Head Neck Surg 2021;73:188ŌĆō92. https://doi.org/10.1007/s12070-020-02329-3.



5. Muhleman MA, Wartmann CT, Hage R, Matusz P, Shoja MM, Tubbs RS, Loukas M. A review of the tragal pointer: anatomy and its importance as a landmark in surgical procedures. Folia Morphol 2012;71:59ŌĆō64.
6. Witt RL, Weinstein GS, Rejto LK. Tympanomastoid suture and digastric muscle in cadaver and live parotidectomy. Laryngoscope 2005;115:574ŌĆō7. https://doi.org/10.1097/01.mlg.0000161343.85009.4c.


7. Ru JA, Benthem PP, Bleys RL, Lubsen H, Hordijk GJ. Landmarks for parotid gland surgery. J Laryngol Otol 2001;115:122ŌĆō5. https://doi.org/10.1258/0022215011907721.


8. Saha S, Pal S, Sengupta M, Chowdhury K, Saha VP, Mondal L. Identification of facial nerve during parotidectomy: a combined anatomical & surgical study. Indian J Otolaryngol Head Neck Surg 2014;66:63ŌĆō8. https://doi.org/10.1007/s12070-013-0669-z.



9. Brintnall ES, Tidrick RT, Huffman WC. A simplified and rapid anatomical approach to parotidectomy. AMA Arch Surg 1955;71:331ŌĆō6. doi:10.1001/archsurg.1955.01270150025002.


10. Zhong W, Ashwell K. Facial nerve trunk variations with sur┬Łgical implications: A cadaveric study. International Journal of Surgery Open 2015;1:35ŌĆō40. https://doi.org/10.1016/j.ijso.2016.02.011.

11. Meybodi AT, Moreira LB, Lawton MT, Preul MC. Anatomical assessment of the digastric branch of the facial nerve as a landmark to localize the extratemporal facial nerve trunk. Surg Radiol Anat 2019;41:657ŌĆō62. https://doi.org/10.1007/s00276-019-02222-x.


12. Kanatas AN, McCaul JA. Use of digastric branch of the facial nerve for identification of the facial nerve itself in parotidectomy: technical note. Br J Oral Maxillofac Surg 2011;49:493ŌĆō4. https://doi.org/10.1016/j.bjoms.2010.10.019.


13. Borle RM, Jadhav A, Bhola N, Hingnikar P, Gaikwad P. Borle's triangle: A reliable anatomical landmark for ease of identifi┬Łcation of facial nerve trunk during parotidectomy. J Oral Biol Craniofac Res 2019;9:33ŌĆō6. https://doi.org/10.1016/j.jobcr.2018.08.004.



15. Righini CA. Facial nerve identification during parotidectomy. Eur Ann Otorhinolaryngol Head Neck Dis 2012;129:214ŌĆō9. https://doi.org/10.1016/j.anorl.2011.12.002.


-
METRICS

-
- 0 Crossref
- 0 Scopus
- 850 View
- 19 Download
- ORCID iDs
-
KangMi Pang

https://orcid.org/0000-0001-9148-9080Su Kyung Kuk

https://orcid.org/0000-0001-9793-2602Eunhye Choi

https://orcid.org/0000-0002-6972-4387 - Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print